|
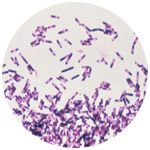
b. Clostridium difficile
|
|
C difficile (C diff) is a major cause of hospital-acquired infectious diarrhea and is associated with increased healthcare costs, prolonged hospitalizations, and higher patient morbidity. Both C diff toxins A and B play a role in the pathogenesis of the infection (Ananthankrishnan 2011). C diff and associated antibiotic therapy have been implicated in the development of enterocolitis, which can be fulminant and result in death. It is an anaerobic spore-forming bacillus and produces a pseudomembranous colitis. Previous antimicrobial use, especially clindamycin or ciprofloxacin, is a risk factor for development of C diff–associated diarrhea (CDAD) by disrupting normal bowel flora and promoting C diff overgrowth (Centers for Disease Control and Prevention 2008). Historically, CDAD has been associated with hospitalized elderly patients or long-term care facility (LTCF) residents. Since 2000, a strain of C diff has been identified as a North American pulsed-field type 1 (NAP1). This strain produces an extra toxin (binary toxin), and is the cause of increased morbidity and mortality among hospitalized patients (Centers for Disease Control and Prevention 2008). In the United States, C diff infections among hospitalized children is also on the rise (Nylund et al. 2011). Patients with vancomycin-resistant C diff infections, especially with diarrhea, have been found to have significant levels of environmental contamination (Sethi et al. 2009). Rifampin-resistant C diff has been found in a US hospital with 37% of recovered isolates and 82% of clone isolates resistant (Curry et al. 2009). Relapse following treatment with metronidazole or vancomycin occurs in 20% of first-time cases, increasing to 40% to 60% in subsequent recurrences (Kelly and LaMont 2008). MDR C diff strains have also been identified in hospital and chronic care facility settings. Guidelines for handling outbreaks of C diff in a healthcare setting include:
-
Visitors and HCWs should be instructed to wash their hands with soap (or antimicrobial soap) and water after being in contact with or caring for patients with C diff infection (CDI)
-
For contact with all body substances, gloves are recommended
-
Disposable thermometers are preferable to electronic thermometers. In areas of increased CDI transmission, chlorine-containing cleaning agents or other sporocidal agents (such as paracetic acid) should be used to disinfect surfaces (Oie et al. 2011)
-
Antimicrobial usage should be monitored, and stewardship efforts should especially focus on antimicrobial drugs associated with a high risk for CDI, especially clindamycin, cephalosporins, and fluoroquinolones
-
Treatment of asymptomatic carriers is not recommended
Use of probiotics to treat C diff carriers and CDI patients remains controversial (Hsu et al. 2010).
|



